PHARMACY CORNER
Healthy Travels

By Stephanie Simons,
Head Pharmacist,
Lindo’s Pharmacy in Devonshire
Bermudians are travellers. We like to get off the Island and explore the world. But the disruption to routine; change in diet, drinking water and climate; different sleep patterns; and new activities can all contribute to possible health issues. Whether you are returning to favourite haunts or discovering new lands, you don’t want to get sick, and there are some simple ways to protect against common travel illnesses.
Before you leave, stay healthy, exercise regularly, eat a balanced diet and get plenty rest. If there will be a time change at your destination, try to gradually shift your schedule to match it.
Research your destination to find out what travel immunizations you should get and what vaccine-preventable diseases you should prepare for.
If you will be visiting a country that requires vaccinations, ensure that you get them in plenty of time. Check the Bermuda Government website at gov.bm/health-clinics-bermuda or call 278-6460 or 278-6461 for more information regarding any required vaccinations for the area you are visiting and when they need to be gotten. There is also a trip planning questionnaire that can be downloaded and completed before your visit to the travel clinic.
Travel from Bermuda often requires at least one flight. In the air, drink plenty of water, eat regularly and avoid alcohol, caffeine or large meals. If you are on a long flight, get up and walk around the plane every hour or two to prevent blood clots.
If your trip takes you across several time zones, you could suffer from fatigue, poor concentration, disturbed sleep, an overall feeling of unwell and even diarrhea or constipation due to jet lag. These symptoms can last for several days: up to one day for every hour difference in time. To avoid having jet lag ruin your plans, adjust your meals and sleep schedule to local time as soon as you arrive. Exercise, eat healthy foods and drink plenty of water. Take a hot, relaxing bath before bed and sleep in a dark and quiet room. If sleep is still a problem, taking melatonin one to two hours before bed can help.
Those who suffer from motion sickness know that it can make travel miserable. If you are prone to motion sickness, move your head as little as possible during travel, don’t eat or drink and avoid reading or watching videos. On a plane, try to sit over the wings; if you are on a cruise, try to get a central cabin; sit in the front seat in a car. Many travellers find that a scopolamine patch placed behind the ear helps to limit the effects of motion sickness. Other remedies include Gravol or other anti-nausea medication, including natural ginger tablets. Some people find that acupressure wristbands can help to ease symptoms. According to the CDC, traveller’s diarrhea is the top travel related illness around the world and affects up to half of all travellers. Fortunately, it is also avoidable. Avoid tap water and ice; canned or bottled drinks are the safest bet. Food should be fresh, fully cooked and eaten hot. Don’t purchase food from street vendors and never eat raw or undercooked meat or seafood. Peel fruits and vegetables yourself. And always keep hands clean with soap and water or an alcohol-based sanitizer, and keep hands away from your face and mouth.
According to the CDC, traveller’s diarrhea is the top travel related illness around the world and affects up to half of all travellers. Fortunately, it is also avoidable. Avoid tap water and ice; canned or bottled drinks are the safest bet. Food should be fresh, fully cooked and eaten hot. Don’t purchase food from street vendors and never eat raw or undercooked meat or seafood. Peel fruits and vegetables yourself. And always keep hands clean with soap and water or an alcohol-based sanitizer, and keep hands away from your face and mouth.
Despite your best efforts you could still get diarrhea, so pack an antidiarrheal medicine such as Imodium, Kaopectate or Pepto-Bismol just to be safe.
Before you leave, throw a few other items into your suitcase that could help to keep you comfortable while away from home: an antihistamine, like Benadryl or Piriton; a hydrocortisone cream such as Cortizone-10; a pain reliever like Advil, Tylenol or Aspirin; a laxative such as Metamucil or Dulcolax; sunscreen; insect repellant with DEET; antacids; and eye drops are a few common travel items.
As you take to the road this summer, take some easy precautions to avoid becoming ill. Stay healthy while you wander the globe and have fun! Bon voyage!
Stephanie Simons is the head pharmacist at Lindo’s Pharmacy in Devonshire. She earned her Bachelor of Science in Pharmacy at Massachusetts College of Pharmacy and has been practicing for over 20 years. She is a registered pharmacist with the Bermuda Pharmacy Council and is a member of the Bermuda Pharmaceutical Association.
First Steps in First Aid

By Stephanie Simons,
Head Pharmacist,
Lindo’s Pharmacy in Devonshire
First aid is the act of helping a person who has become suddenly sick or injured. We will all require – or administer – first aid at some point: it’s part of life’s unexpected bumps and scrapes along the way.
Anyone is able to give first aid. In fact, the majority of those who help with first aid are simply people who happen to be nearby.

Serious injuries require medical assistance. Dial 911 for assistance.
The best way to approach first aid is to stop, take a deep breath and assess the situation. Do not put yourself in danger, and if the injured or ill person is in danger, remove them if they can be moved. Always wash your hands before and after giving first aid and wear gloves if available.
Serious injuries require medical assistance but there are many common injuries that can be treated with basic first aid.
Cuts and scrapes
Apply pressure with a clean cloth or dressing to stop the bleeding. Once bleeding stops, clean the wound and remove any debris with tweezers. Apply an antibiotic such as Neosporin or Polysporin and cover with a bandage.
Stings
Provided the person is not allergic to an insect sting, simply remove the stinger by scraping across the skin with a fingernail or credit card. Stings from plants such as poison ivy require immediate and thorough washing. As a rash appears, apply a cold compress to alleviate discomfort and administer antihistamine such as Benadryl or Piriton. For both plant and insect stings, apply Calamine lotion or hydrocortisone cream such as Cortizone-10 or a generic Hydrocortisone Cream to the site.
Burns
Immediately hold a burn under cool running water, or apply a cool, wet cloth. Cover blisters with a loose gauze. Do not break blisters; if they break on their own, apply an antibiotic cream like Polysporin.
Shock
An injured person might show signs of shock, such as pale, clammy skin, rapid breathing, dizziness or nausea or vomiting. If you suspect a person might be in shock, lay them down and elevate their legs. Keep the person still, loosen their clothing and cover with a blanket. Stay with them until help arrives.
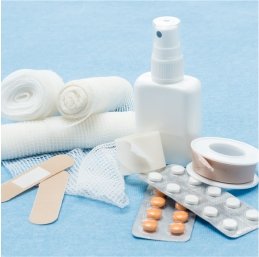
A well-stocked first aid kit is a necessity.
An important tool in first aid is a properly equipped first aid kit. For personal use, a first aid kit should be kept at home, in the car, on your boat or anywhere else you spend time. Also be aware of where first aid kits are stored at work, your gym or other places you regularly visit. And keep one in your suitcase for travel.
It is easy and inexpensive to assemble your own first aid kit. Use any bag that will allow items to be visible and easily accessible, such as a make-up bag or a clear plastic container with a lid. Sort items according to type and organize in re-sealable plastic bags. A first aid kit should contain at least the following items:
- Adhesive and non-stick bandages in various sizes
- Sterile gauze pads in various sizes
- Adhesive first aid tape – waterproof or cloth
- Tweezers to remove dirt, splinters or thorns
- Antiseptic wipes or spray, such as Bactine or Dettol
- Hydrocortisone cream and antibiotic cream such as Neosporin, Polysporin
- Pain relievers such as Ibuprofen (Advil), Acetaminophen (Tylenol) or Aspirin (do not give Aspirin to children)
- Thermometer
- Antihistamines like Benadryl, Piriton or Claritin for allergic reactions
- Absorbent compress dressings
- Elasticized (Ace) bandage for support for sprains
- Instant cold compress (or, if at home, an ice pack in the freezer)
If family members have specific needs such as prescribed medication, store that in the kit as well. Other good additions are a flashlight, latex or rubber gloves and hand sanitizer. Check your kit every six months for expiration dates.
With any luck, your first aid kit will sit untouched. But when mishaps occur, a properly stocked kit and some basic first aid knowledge can come to the rescue.
Stephanie Simons is the head pharmacist at Lindo’s Pharmacy in Devonshire. She earned her Bachelor of Science in Pharmacy at Massachusetts College of Pharmacy and has been practicing for over 20 years. She is a registered pharmacist with the Bermuda Pharmacy Council and is a member of the Bermuda Pharmaceutical Association.
Nip Seasonal Allergies in the Bud

By Stephanie Simons,
Head Pharmacist,
Lindo’s Pharmacy in Devonshire
Spring is officially here, bringing us longer days, warmer weather, fragrant flowers, and those dreaded seasonal allergies. Itchy, watery, red eyes, sneezing, itchy throat, congestion and a runny nose are just a few of the symptoms that those with seasonal allergies may suffer from at this time of the year. The good news is that the symptoms are manageable, so to keep the ‘spring’ in your step let’s look at what can cause these allergies, and how we can all nip them in the bud.
What Causes Seasonal Allergies?
Seasonal allergies, also known as hay fever and allergic rhinitis, typically occur between March and May. They are caused by triggers or allergens that are carried in the air. Grass, pollen and mold are the most common causes, but in Bermuda, the main culprits at this time of the year are cedar trees, casuarina trees, rye grass and Bermuda grass. The reason that these plants can cause allergies to flare up is because of the way that they reproduce. Instead of relying on birds and insects to carry their pollen, they produce large amounts of tiny, wind-borne pollen.
The island’s warm and humid climate is also the perfect breeding ground for mold. Much like pollen, outdoor mold spores release into the air. Once airborne, the pollen and mold spores can get into our eyes, noses, skin, clothes, and into our houses. Keep in mind that pollen counts thrive during cool nights, warm days, and after rainfall. read more…
TOP NUTRITION TIPS

By Stephanie Simons,
Head Pharmacist,
Lindo’s Pharmacy in Devonshire
It’s March, which means that it is National Nutrition Month. It’s a great time to focus on ways that you can ensure you are getting the daily nutrients you need and more for optimal health.
However, this month brings awareness to much more than what we should and shouldn’t eat. Let’s break it down with some top tips to combine good nutrition and a healthy lifestyle.
Get outside more.
The weather is warming up now and we are gearing up for summer. If you have been inside most of the winter, or if you have a job that keeps you in an office all day, it’s time to get yourself outside to enjoy some of Bermuda’s national parks.
Take a bike ride or a walk along the railway trails, feel the sand between your toes at a beach you haven’t been to in a while, explore Tom Moore’s jungle or climb the lighthouse for a spectacular view of our island.
Adults should aim for 30 minutes of moderate-intense activity five times per week. If you are busy, you can spread it out throughout the day by doing ten minutes at a time. Lunch breaks are the perfect excuse for a walk, or even a few light stretches to ease any tension from sitting at a desk.
Fitness events are a great way to get motivated. The Lindo’s to Lindo’s 5K run and 4-mile walk is coming up on Sunday, March 13. For more information on how to sign-up, visit the Lindo’s website: https://lindos.bm/lindos-10k-run-4-mile-walk-2016/.
Take a break.
Did you know that how, when, why and where you eat are just as important as what you eat? Take the time to enjoy your surroundings while you eat, and you will enjoy your food even more. At times it is impossible to avoid eating on-the-go, but generally you should avoid multitasking while you eat. read more…
Improve Your Oral Health to Help Prevent Disease

By Stephanie Simons,
Head Pharmacist,
Lindo’s Pharmacy in Devonshire
February is Oral Health month, a month set aside to spread awareness of chronic mouth pain, throat cancer, oral sores, birth defects of the lip and palate, gum disease, tooth decay and all other diseases relating to the oral cavity. Clearly, oral health includes a variety of ailments. In this article, I will focus on the things we all can do to improve our oral health, in an effort to stave off disease.
Cavities
Perhaps the most well-known and most prevalent oral ailment is a cavity. Cavity is a term for tooth decay, which results from bacteria. The mouth is commonly filled with bacteria that mix with saliva to form plaque on the teeth. Plaque is removed by brushing your teeth, but in the event that it is not removed, the acids in plaque damage the enamel protecting the teeth. This can create holes in the teeth, known as cavities, which lead to tooth decay.
Symptoms
Cavities are visible to the eye and range from yellow to black. Small cavities may not hurt, but large ones, especially those affecting nerves, are painful. Cavities are diagnosed by a dentist, which is why regular visits to a dental hygienist is important.
Prevention
Diet plays a role in oral health. Having a well-balanced diet helps prevent tooth decay. As importantly, decreasing your sugar intake will help avoid the formation of cavities. Likewise, sticky foods are more harmful as they remain on the teeth longer. However, dental cavities can be prevented by regularly brushing and flossing, and using toothpaste with fluoride.
Treatment
Treatment for cavities require a visit to the dentist and include fillings, crowns and/or root canals. Fillings, as the name implies, involves removing all decay from the tooth with a drill and filling the space, for example with gold, silver alloy or porcelain. Crowns, also known as caps, are used in more serious cases where the majority of the tooth is weak. Here, a fitted crown or cap, usually made of gold or porcelain, is placed over the teeth. For cavities that result in nerve injury or decay, a root canal is required. This involves removing the centre of the tooth, including the nerve and filling the root with a sealing material. Root canals often are accompanied by crowns. read more…
Supplement Your Diet with Vitamins to Meet Your Nutrition Needs

By Stephanie Simons,
Head Pharmacist,
Lindo’s Pharmacy in Devonshire
The start of the New Year brings with it a slew of New Year resolutions. Many of these are focused on living a healthier life, be it with exercise or diet. These are noble goals that should be aspired to all year long. As the year unfolds, however, busy schedules can make resolutions hard to follow every day. When it comes to getting the nutrients you need, multivitamins can help fill the gaps in your diet.
What is a Multivitamin?
A multivitamin, as the name implies, is a supplement that contains various vitamins, minerals and nutrients. Multivitamins are available in a number of forms, including but not limited to a pill, liquid, powder and injection. Typically to qualify as a multivitamin, there needs to be at least three different vitamins or minerals included in the formulation.
For multivitamins that are available over the counter, each vitamin and mineral component is at a level below the maximum tolerable level determined by the U.S. Food and Drug Administration. There are multivitamins that include very high doses of certain vitamins, minerals and nutrients. Prescription vitamins are available for individuals who need a particularly high dose of a certain vitamin or mineral.
Why Consider Taking a Multivitamin?
Getting the recommended dosage of nutrients, minerals and vitamins is an important part of being healthy and it can be difficult through diet alone. Multivitamins can help fill the gaps in the diet so that the body has access to all the elements it needs to thrive.
The most recent Dietary Guidelines for Americans issued by the U.S. Department of Agriculture and the U.S. Department of Health and Human Services in 2010 report that calcium, vitamin D, dietary fibre, and potassium intake in adults and children is so low that it qualifies as a public health concern. A supplement could help to fill the nutritional void in these areas.
Taking a multivitamin is easy and does not require a heavy time commitment. It can be as easy as taking one pill in the morning every day.
Who Should Take Multivitamins?
Anyone seeking to complement his or her diet with the recommended intake of vitamins, minerals and nutrients should consider incorporating a multivitamin into their routine. For individuals with specific medical needs, speak to a physician or pharmacist about what multivitamins are good for you.
In addition, certain groups need increased vitamin levels. For example, The United Kingdom Food Standards Agency (FSA) recommends that pregnant women take an increased dose of folic acid and iron. The FSA has also adviced that elderly people may benefit from additional vitamin D and iron. There are special multivitamins that are targeted to these groups of people. Likewise, there are multivitamins specifically targeted for men, women and children and these supplements have varied percentages of vitamins, minerals and nutrients based on the needs of its target population.
What is the Recommended Intake?
Multivitamins are not a replacement for eating healthy, but rather a supplement to a healthy diet. For people with strict diets that limit certain foods, a multivitamin also can supplement the missing nutrients. As multivitamins vary between types and brands, review the dosage information that comes with the multivitamin to determine how often and when to take it.
What are the Risks Associated with Taking a Multivitamin?
While the body needs nutrients, overdosing on a vitamin can result in negative side effects. This is why it is important to follow the recommended dosage when taking a multivitamin. If multiple supplements are being taken together, it is especially important to compare ingredients to avoid excess intake of any particular nutrient. When in doubt, speak to your pharmacist about how to take your vitamins.
Which Multivitamin is Right for You?
As noted above, there are multivitamins targeted to specific populations, such as for children, the elderly and pregnant women. There also are multivitamins specifically designed for either men or women. When selecting your multivitamin, be sure to select one that matches your demographic.
Since most of us do not know the exact amounts of each vitamin or mineral that our body needs, multivitamin labels include for each of its components the per cent of recommended daily value. In other words, if an element is included at 100 per cent of the daily recommended value, then that supplement will provide you with the full amount needed in one day for that specific component. Some multivitamins include more than 100 per cent of the recommended daily value for certain nutrients or vitamins. Ultimately, this is unnecessary and those multivitamins with 100 per cent are sufficient. Keep in mind that certain components such as calcium and magnesium are rarely included at 100 per cent of the daily value as it would make the multivitamin too large in size to swallow comfortably.
Where Are Multivitamins Available?
Multivitamins are available at the pharmacy and come in a wide array of options. Visit Lindo’s pharmacy to find the multivitamin of your preference. If you have any questions, speak with a pharmacist who can help you decide what is best for you.
Stephanie Simons is the head pharmacist at Lindo’s Pharmacy in Devonshire. She earned her Bachelor of Science in Pharmacy at Massachusetts College of Pharmacy and has been practicing for over 20 years. She is a registered pharmacist with the Bermuda Pharmacy Council and is a member of the Bermuda Pharmaceutical Association.
How to Protect Yourself from Influenza this Holiday Season

By Stephanie Simons,
Head Pharmacist,
Lindo’s Pharmacy in Devonshire
Influenza is an infectious disease that spreads easily from one person to another. With the holidays ahead, it is important that you know the facts about influenza so that you can stay safe and help prevent the spread of disease.
Seasonal influenza, commonly known as “flu”, is an acute infection that is caused by the influenza virus, which has three subtypes: A, B and C. Within each subtype, there are several strains that change from year to year. Types A and B are the most frequent viral subtype and these are the strains found in the seasonal influenza vaccines.
According to the Centers for Disease Control and Prevention (CDC), seasonal influenza peaks between October and May in temperate climates. The severity and nature of the flu changes from year to year.
Prevalence
Every year, approximately 10 per cent of adults and up to 30 per cent of children have influenza. Each year, there are up to 500,000 deaths that result from influenza and up to 5 million cases are considered severe.
Vaccination
The World Health Organisation (WHO) recommends annual vaccination against seasonal influenza. For high risk individuals and people who spend time with anyone in this population, vaccination is especially important to prevent contamination and the complications associated with the disease. The vaccine has been shown to be safe and has been used for more than 60 years. The effectiveness of the vaccine is dependent on which strains of the virus are circulating in any particular influenza season. Since 2013, there has been a quadrivalent vaccine available that includes protection against two influenza A strains and two B strains. Prior to this, trivalent vaccines only protected against two A strains and one B strain.
Signs and Symptoms
Since seasonal influenza peaks in the winter months, it is important that you know the signs to look out for and how to differentiate between the flu and the common cold. Seasonal influenza typically presents itself with the onset of a high fever, dry cough, headache, muscle and joint pain, sore throat, runny nose and general discomfort. The incubation period for influenza is approximately two days, which means that it usually takes two days between the time of infection and the onset of the disease.
The common cold also is caused by a virus, albeit a different one from influenza. Though symptoms are similar, colds are less severe than influenza and generally do not lead to complications like pneumonia, infection and hospitalisation as does the flu. Runny and stuffed noses are common symptoms for the cold, while influenza is often associated with stronger body aches, fever, extreme fatigue and dry cough. Your doctor can run tests to determine the specific viral infection.
Treatment
The prescription treatments for seasonal influenza are known as antiviral drugs and for best results, they should be taken within 48 hours of the first symptom. Non-prescription treatments include lots of rest and fluids. Treat the symptoms that are most bothersome – pain relievers for body aches and fever, cough syrups for that annoying cough and so on.
Risks
Influenza ranges from mild to severe and in the worst cases can lead to hospitalisation and even death. Individuals at high risk for severe influenza include children aged under 2 years, adults aged 65 years or older, pregnant women and individuals with weakened immune systems or with chronic heart, lung, kidney, liver, blood or metabolic diseases. It is important for this population to seek medical attention at the earliest sign of symptoms. It is especially recommended that this group be vaccinated against influenza, when possible.
The Spread of Disease
As previously noted, influenza is an infectious and contagious disease. It is also an airborne disease, which means that it is spread through infected particles in the air. When an infected person coughs, the virus can infect others who breathe in the particles.
The virus can also be spread by hand contamination. We are taught to use our hands to contain a cough or sneeze. As a result, infected particles land on hands and can be transmitted to others through contact.
Preventing the Spread of Disease
People with seasonal influenza should stay at home. The disease is very contagious and easily spreads. To avoid contaminating schoolmates, co-workers and the community, the best thing someone with influenza can do is to remain isolated from others.
If you are unsure if you have influenza, see a medical professional who can diagnose the disease. In the meantime, when coughing or sneezing, always use a tissue and be sure to wash your hands regularly.
Preventing the Disease
The best way to prevent the flu is to keep healthy. Eat a balanced diet, increase your vitamin C intake and if you take supplements take immune system boosters like Echinacea.
If you fall in the higher risk category make sure you get vaccinated against the flu.
Stephanie Simons is the head pharmacist at Lindo’s Pharmacy in Devonshire. She earned her Bachelor of Science in Pharmacy at Massachusetts College of Pharmacy and has been practicing for over 20 years. She is a registered pharmacist with the Bermuda Pharmacy Council and is a member of the Bermuda Pharmaceutical Association.
Diabetes Awareness

By Stephanie Simons,
Head Pharmacist,
Lindo’s Pharmacy in Devonshire
November 14 is World Diabetes Day. We take this opportunity to educate the public about this chronic disease. Last year, there was a reported 6,900 cases of diabetes in Bermuda, according to the International Diabetes Federation (IDF). This is nearly 10 per cent of the population in Bermuda, and the number of cases is expected to rise in the coming years. In fact, the IDF estimated that in 2014, there were an additional 1,900 undiagnosed cases of diabetes in Bermuda.
The prevalence of diabetes in adults is higher in Bermuda than it is around the world. This is a result of our lifestyle and we need to make a serious change to improve the health of our community. To start, we must understand this disease, its risks, symptoms, treatment and how best to prevent its onset.
Diabetes & Its Implications
 Diabetes results from the body’s inability to produce or process the hormone insulin. During digestion, the carbohydrates we eat are broken down into the simple sugar known as glucose. Insulin helps regulate the level of glucose in our blood, so that our bodies can produce energy from the foods that we eat. In people with diabetes, glucose levels are not managed naturally and this may lead to serious health complications, including heart disease, kidney failure and blindness. Worldwide, diabetes results in almost five million deaths each year. read more…
Diabetes results from the body’s inability to produce or process the hormone insulin. During digestion, the carbohydrates we eat are broken down into the simple sugar known as glucose. Insulin helps regulate the level of glucose in our blood, so that our bodies can produce energy from the foods that we eat. In people with diabetes, glucose levels are not managed naturally and this may lead to serious health complications, including heart disease, kidney failure and blindness. Worldwide, diabetes results in almost five million deaths each year. read more…
Healthy Seniors

By Stephanie Simons,
Head Pharmacist,
Lindo’s Pharmacy in Devonshire
When we reach our 60s, 70s and beyond, it doesn’t mean that we can’t enjoy life as much as, or even more than, we did in our youth. We have more time, more wisdom and greater perspective than ever before and we need to stay healthy and enjoy it!
True, genetics can predetermine some of how we age, but for the most part we can control many of the factors that affect us over time. Many are simple lifestyle choices that can enable us to be healthy and happy seniors.
Physical Health
As we age, bones lose density, which makes them weaker and more prone to fracture, muscles lose strength and flexibility, and cartilage wears down. This leads to loss of strength and poor balance, and falls that can result in injury become a concern.
To compensate for some of these changes, women over 50 and men over 70 should increase calcium from 1000mg a day to 1200mg a day. Vitamin D should also increase from 600IU to 800IU for adults over 70.
A healthy diet of vegetables, fruits, whole grains, high fibre, lean protein and limited saturated fat and sodium provides a substantial amount of these and other vitamins and minerals that our bodies need. It can help us to lose weight if necessary and maintain a healthy weight. Proper eating can also manage disease such as heart disease, high blood pressure, diabetes and some cancers. read more…
Prostate and Ovarian Cancer Awareness Month

By Stephanie Simons,
Head Pharmacist,
Lindo’s Pharmacy in Devonshire
Prostate and ovarian cancers are a scary diagnosis. This month, we are focusing on these types of cancer to ensure both men and women are aware of the symptoms and risks.
Ovarian cancer is known as the “silent killer” as many women don’t know they have it until the advanced stages. Prostate cancer is similar in that there are no early warning signs and without regular screenings, it can go undetected for years.
Let’s discuss ovarian cancer first. What is it? According to Target Ovarian Cancer, the UK’s leading ovarian cancer charity, it arises from the cells in and around the ovaries which are two small organs located low in the tummy just above the pubic area. They form part of a woman’s reproductive system, storing eggs which are released into the womb for fertilisation. The ovaries also are responsible for making the hormones estrogen and progesterone. Sometimes cells around these organs can form tumours, and in some of these cases, the tumours are cancerous. Post-menopausal women in particular need to watch out for symptoms that might indicate a type of ovarian cancer.
Some of the symptoms that should be watched include:
- Persistent pelvic or abdominal pain
- Increased abdominal size/persistent bloating – not bloating that comes and goes
- Difficulty eating or feeling full quickly
- Needing to urinate more urgently or more often than usual
If you have any of these symptoms and they aren’t normal for you, visit your doctor as soon as possible. Some of the risks include age, family history, weight, use of Hormone Replacement Therapy, ovarian cysts and endometriosis. But the good news is, you can reduce the risks by using the combined contraceptive pill, having children and breastfeeding them and living a healthy lifestyle with regular exercise.
Now let’s talk prostate cancer. According to the American Cancer Society’s Cancer.org, prostate cancer begins in the gland cells of the prostate, which is found only in males.
The exact cause of prostate cancer is unknown. The only confirmed factors currently known to increase one’s risk for prostate cancer are family history, age, African-American ethnicity, diet and chemical exposure.
Common symptoms include:
- Frequent urination (especially at night)
- Weak urinary stream or an inability to urinate
- Interruption of urinary stream (stopping and starting)
- Pain or burning on urination
- Blood in the urine or ejaculate
- Bone pain in the hips, ribs or general back pain
- Back pain
Because there are no early warning signs for prostate cancer, and sometimes there aren’t any noticeable symptoms, men can undergo a screening for the disease. Screenings do not provide a diagnosis, but they provide valuable information in finding the disease early. Screening commonly involves two tests: the prostate specific antigen (PSA) blood test, and the digital rectal exam (DRE).
While there’s no sure way to prevent prostate cancer, there are ways to reduce your risk. In general, doctors recommend that men with an average risk of prostate cancer make choices that benefit their overall health if they’re interested in prostate cancer prevention. Preventative measures include choosing a healthy diet, maintaining a healthy weight, exercising most days of the week and discussing risks with your doctor. These aren’t guaranteed to decrease your risk of prostate cancer, but making these choices will benefit your overall health.
The key with both of these cancers is to know how to minimize risks, understand symptoms and schedule an appointment with your doctor as soon as possible so that diseases don’t go undetected. Early detection can save a life. The Bermuda Cancer and Health Centre also is a resource for a range of screening services, support and educational programs at 441-236-1001 or www.cancer.bm.
Stephanie Simons is the head pharmacist at Lindo’s Pharmacy in Devonshire. She earned her Bachelor of Science in Pharmacy at Massachusetts College of Pharmacy and has been practicing for over 20 years. She is a registered pharmacist with the Bermuda Pharmacy Council and is a member of the Bermuda Pharmaceutical Association.



